Our Approach
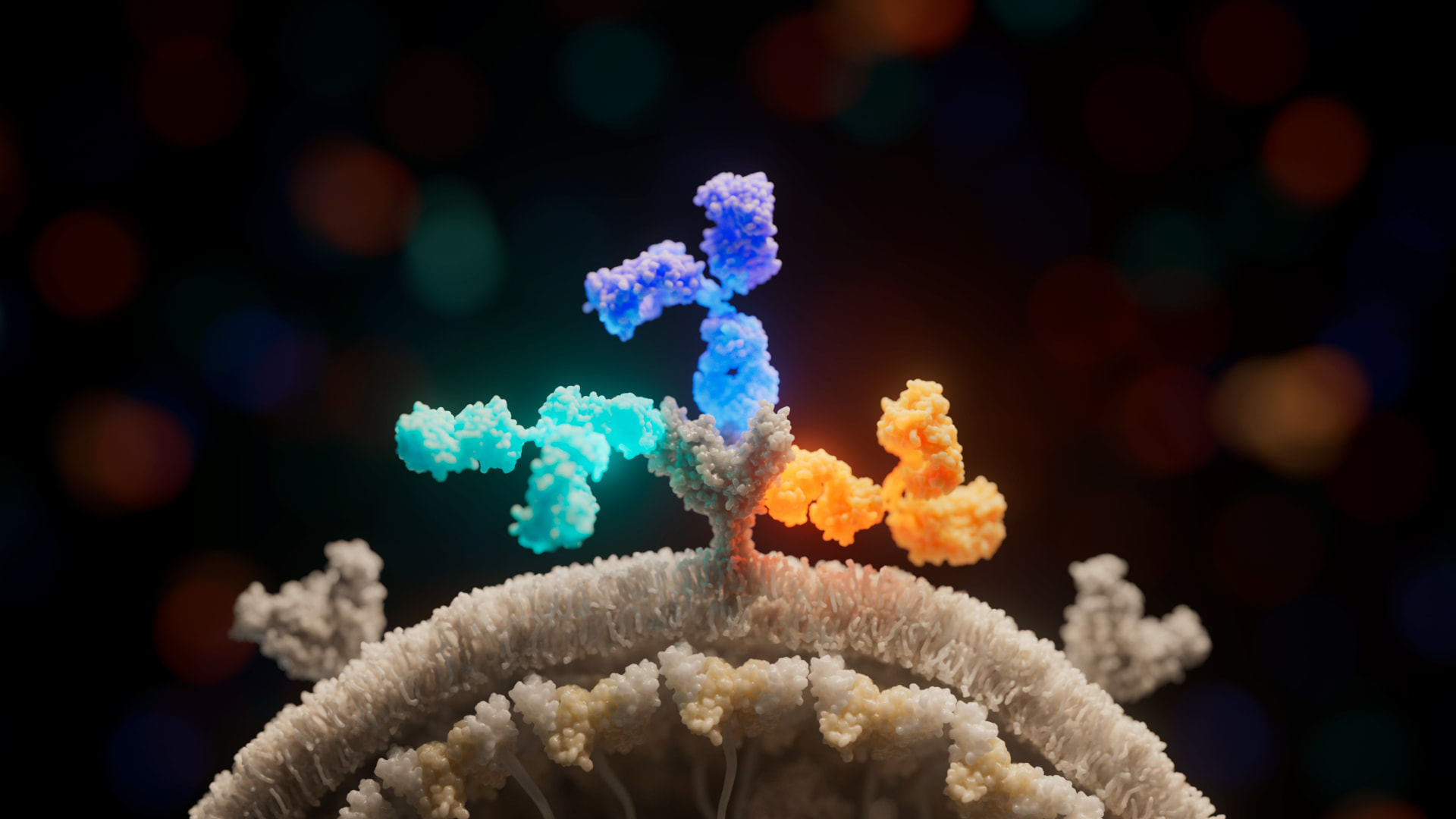
Structural biologist Erica Ollmann Saphire, Ph.D., has solved the structure of various Ebola proteins to understand how they could be targeted by antibodies. In a series of groundbreaking discoveries beginning a decade ago, her team determined the molecular structures of surface glycoproteins essential for invasion of human cells by Ebola, Sudan, Bundibugyo and Marburg viruses—each interacting with a patient-derived antibody recognizing that virus. These analyses now serve as blueprints for regions on the virus’ outer glycoprotein that could be targeted by antibodies to halt viral infection. This work also guides clinical development of “neutralizing” antibodies that could be infused into patients already infected with the virus. In fact, in 2014, Dr. Saphire and her colleagues were the first to show how an experimental Ebola virus therapy used an antibody “cocktail” to combat infection.
An internationally-known expert in the field, Dr. Saphire has made the La Jolla Institute for Immunology home to the Viral Hemorrhagic Fever Immunotherapeutic Consortium (VIC), a coalition of 45 previously-competing labs across five continents. This pioneering group is working to define which therapeutic antibodies effectively combat Ebola virus and related pathogens. Under Dr. Saphire’s leadership, the VIC has pooled the expertise of structural biologists, virologists, immunologists, clinicians, and public health practitioners to advance new therapies and vaccines faster than ever before.
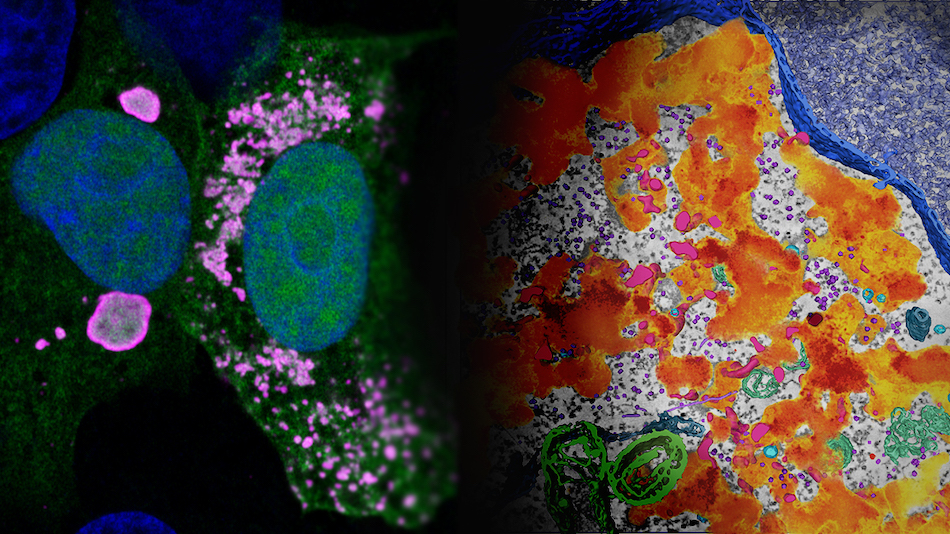
Dr. Saphire has established a molecular imaging facility at LJI for cryo-electron microscopy (cryo-EM). Through cyro-EM, researchers at LJI can quickly produce extremely detailed images of viral structures and reveal vial targets that could be neutralized by human antibodies or drug therapies.
This new equipment, along with Dr. Saphire’s expertise, has driven advances in structural biology and unlocked new strategies against Ebola virus. In 2022, Dr. Saphire’s lab published a collaboration with Scripps Research scientists showing how a human protein in Ebola-infected cells actually starts helping the virus. This work suggests targeting this process may slow Ebola’s ability to make copies of itself and spread through the body. In 2023, the Dr. Saphire Lab published an important investigation into how Ebola virus turns host cells into “virus factories” and churns out new viral particles.
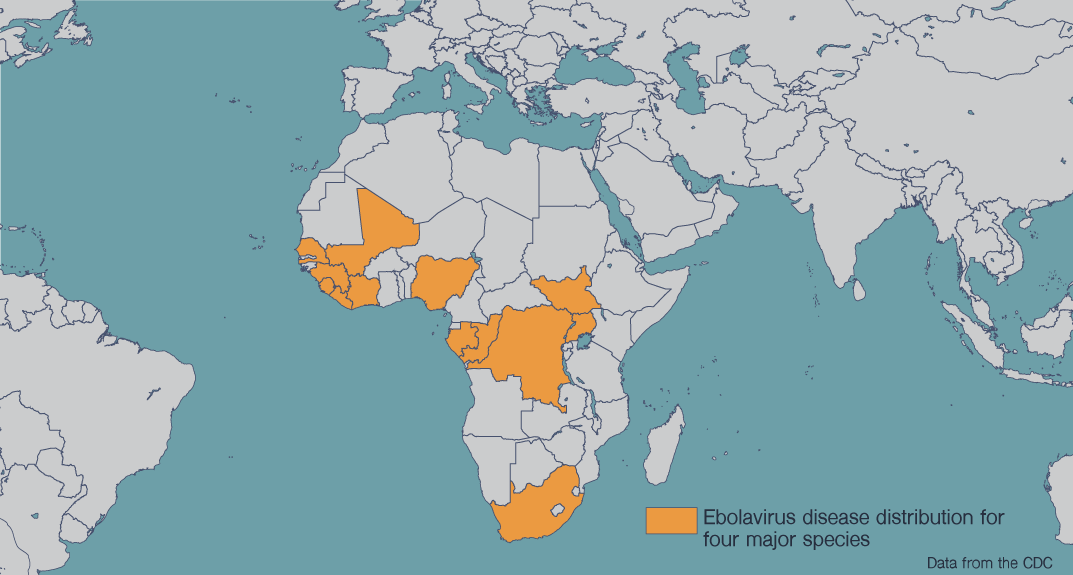
Also in 2022, Dr. Saphire and research partners at Emory University made a major advance in the effort to develop an antibody cocktail against Ebola. The researchers found that human antibodies can target two ebolavirus species at once: Ebola virus and Sudan virus. These two species are responsible for the biggest, deadliest outbreaks of Ebola hemorrhagic fever. The new report suggests researchers could combine these two potent antibodies to make a powerful antiviral therapy.
Research into Ebola virus therapies continues. In 2023, Dr. Saphire and her colleagues shared a closer look at the structure and function of the first FDA-approved treatment (called Inmazeb / REGN-EB3) for Zaire ebolavirus (Ebola virus). The treatment is a three-antibody cocktail designed to target the Ebola virus glycoprotein. The drug was first approved for clinical use in October 2020, but its exact mechanism of action had remained unclear. In a cover story for Cell Host & Microbe, the LJI researchers presented a high-resolution, 3D structure of the three antibodies as they bind to the Ebola virus glycoprotein (the viral protein that launches Ebola virus infection). This model revealed new information about both the drug and the virus, and how their interaction fights infection and protects against future viral mutations.