Highlights:
- Scientists have discovered that protective T cells travel to the prostate to establish residency and guard against infectious disease.
- We may be able to one day harness these same T cells to combat prostate cancer tumors and other prostate maladies.
LA JOLLA, CA — More than 35,000 men in the United States die from prostate cancer each year. Now, a new study reveals the immune cell weaponry we might use to save lives.
Researchers have discovered that the immune system’s T cells can travel to the prostate to provide long-term protection against infections. Their findings suggest we might harness these same disease-fighting cells to treat prostate cancer.
“This study provides a key framework for understanding prostate T cell immunity. Going forward, we are committed to understanding how to leverage these insights in the context of prostate cancer and cancer immunotherapies,” says La Jolla Institute for Immunology (LJI) Assistant Professor Miguel Reina-Campos, Ph.D., co-senior author of the new Immunity study.
“This work illuminates how T cell responses evolve within prostate tissue, demonstrating that where a T cell lives in the tissue shapes its function,” says Ananda Goldrath, Ph.D., Presidential Chair in Molecular Biology at UC San Diego, member of Moores Cancer Center, and co-senior author of the new study. “Defining the T cell niche in prostate tissue reveals strategies to enhance or regulate immunity in the context of infection and malignancy.”
The new study included collaborators at the Allen Institute and the UC San Diego Moores Cancer Center.
The prostate stands guard
Most people think of the prostate as simply part of the male reproductive system, where it produces key components of seminal fluid that support and transport sperm. However, the prostate’s position in the body means it needs to play additional roles. The urethra, which carries urine out of the body, passes directly through the prostate on its way to the penis. Because this shared passage can also serve as a route for pathogens, the prostate functions beyond reproduction.
“The prostate is a barrier tissue that protects the male reproductive system from pathogens,” says Reina-Campos.
Scientists need to know more about how the prostate stays healthy. Not only is prostate cancer common, but around 2 million men in the United States visit the doctor each year due to inflammation of the prostate, called prostatitis, which can cause intense pain and even infertility.
Tracking T cells in action
Reina-Campos and his colleagues, including the study’s lead author, Kennidy Takehara, Ph.D., of the UC San Diego Moores Cancer Center and the Allen Institute, set out to chart exactly how the immune system’s T cells respond to pathogens in the prostate. To do this, the scientists combined some of the newest single-cell technologies available. Their work is part of the growing field of spatial immunology, in which scientists map the exact arrangements of immune cells within specific parts of the body.
The researchers began with experiments in a mouse model, which revealed the presence of T cells in the prostate. These T cells are known as “tissue resident memory T cells,” because they travel to the prostate and then remain in that organ for months or years.
But were these T cells good fighters?
To learn more, the researchers tracked cell activity over time in a mouse model of viral infection. They discovered that once the mouse immune system cleared the virus, it sent a flood of memory T cells down to the prostate. These T cells adapted to life in the prostate and stood ready to fight the virus if it ever came back.
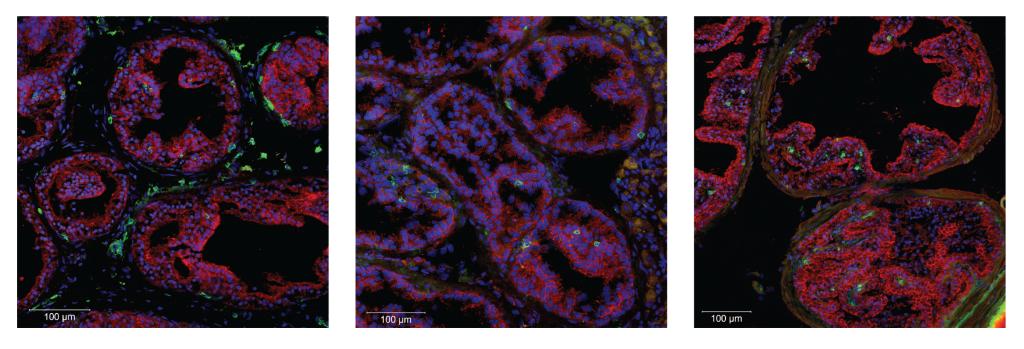
The scientists then examined healthy human prostate tissue, provided by study collaborators at the UC San Diego Moores Cancer Center. The human samples contained tissue-resident memory T cells, similar to those in the mouse model.
“We saw a population of these T cells get deployed to establish full-time residency in the prostate,” says Reina-Campos. “Those T cells live in the prostate for many months for mice—and probably many years for humans.”
Next steps for prostate health

The discovery that T cells travel to the prostate to provide long-term protection counters previous assumptions about immunity in the organ, says Reina-Campos.
Although researchers have found that T cells struggle to enter the prostate to fight tumors, the new study shows T cells can enter the barrier tissue to protect against pathogens,” says Reina-Campos. “This was an overlooked organ, and I hope this study helps reframe it not as immunologically inaccessible, but as a tissue with distinct rules of immune engagement and rich, underappreciated immunobiology.”
The new study brings researchers closer to developing therapies that harness T cells to treat a range of diseases in the prostate.
“Understanding how T-cells behave in this specific tissue will allow us to then tone down inflammatory conditions such as prostatitis, or enhance T cell activity to treat prostate cancer,” says Reina-Campos.
Additional authors of the study, “Distinct tissue niches contribute to prostate tissue-resident memory CD8+ T cell differentiation and heterogeneity,” include study first author Kennidy K. Takehara, Alexander Monell, Vida Luna, Baxter Melisso, Kianoosh M. Mempel, Kitty P. Cheung, Natalie Zane, Peter P. Challita, Amir Ferry, Ethan C. Xu, Violante Olivari, Nicole E. Scharping, Giovanni Galletti, Sara Quon, Julien R. Ishibashi, Nina Estep, John B. Johanneson, Chinmayi Pandya, Stephanie D. Anover-Sombke, Rana R. McKay, Peter J. Skene, Matthew E. Pipkin, and Maximilian Heeg,
This study was supported by a NCI Predoctoral to Postdoctoral Fellow Transition (F99/K00) Award (grant K00CA222711), a Cancer Research Institute Postdoctoral Fellowship (grant CRI4145), and the National Institute of Health (grants R01AI179952, R37AI067545, R01AI072117, R01AI150282, P01AI145815, and F31AI176705.
This work was performed in the context of the immgenT project within the ImmGen consortium, supported by R24072073.